TMD (Temporomandibular Disorders)
On this page
Overview
Temporomandibular disorders (TMDs) are a group of more than 30 conditions that cause pain and dysfunction in the jaw joint and muscles that control jaw movement. “TMDs” refers to the disorders, and “TMJ” refers only to the temporomandibular joint itself. People have two TMJs; one on each side of the jaw. You can feel them by placing your fingers in front of your ears and opening your mouth.
There are three main classes of TMDs:
- Disorders of the joints, including disc disorders.
- Disorders of the muscles used for chewing (masticatory muscles).
- Headaches associated with a TMD.
There are several disorders within each class. See diagram below for some examples.
Classification of Temporomandibular Disorders (TMDs) with Examples
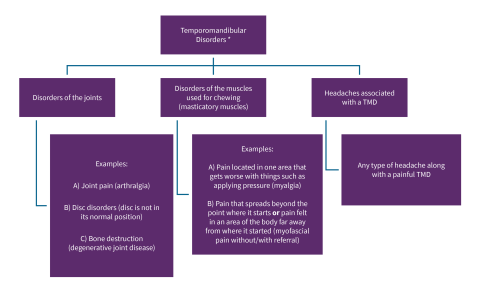
*A person may have one or more of these conditions at the same time.
Many TMDs last only a short time and go away on their own. However, in some cases they can become chronic, or long lasting. In addition, TMDs can occur alone or at the same time as other medical conditions such as headaches, back pain, sleep problems, fibromyalgia, and irritable bowel syndrome.
A recent study found that about 11-12 million adults in the United States had pain in the region of the temporomandibular joint.
Temporomandibular disorders are twice as common in women than in men, especially in women between 35 and 44 years old.
Back to topCauses
Injury to the jaw or temporomandibular joint can lead to some TMDs, but in most cases, the exact cause is not clear. For many people, symptoms seem to start without obvious reason. Recent research suggests a combination of genes, psychological and life stressors, and how someone perceives pain, may play a part in why a TMD starts and whether it will be long lasting.
Because TMDs are more common in women than in men, researchers are exploring whether the differences in TMJ structure and mechanics between females and males may play a role.
Research does not support the belief that a bad bite or orthodontic braces cause TMDs.
Back to topSymptoms
It is important to know that sounds (such as clicking or popping) without pain in the TMJs are common, are considered normal, and don’t need treatment.
However, the following symptoms may signal a TMD:
- Pain in the chewing muscles and/or jaw joint (most common symptom).
- Pain that spreads to the face or neck.
- Jaw stiffness.
- Limited movement or locking of the jaw.
- Painful clicking, popping, or grating in the jaw joint when opening or closing the mouth.
- Ringing in the ears, hearing loss, or dizziness.
- A change in the way the upper and lower teeth fit together.
Diagnosis
There is no widely accepted, standard test available to diagnose TMDs. Because the exact causes and symptoms are not clear, identifying these disorders can be difficult.
Your doctor or dentist will note your symptoms and take a detailed medical history. He or she will ask questions about your pain, including its location, when it occurs, what makes it better or worse, and if it stays in one area or spreads to other parts of your body. The doctor or dentist will also ask if you have other pain conditions such as headache or back pain.
He or she also will examine your head, neck, face, and jaw for tenderness; jaw clicking or popping; or difficulty with movement. The doctor or dentist might also suggest imaging studies such as an x-ray, magnetic resonance imaging (MRI), or computed tomography (CT).
Pain in the mouth, jaw, or face may or may not be related to TMDs. Your doctor or dentist may have to rule out other conditions before diagnosing a TMD.
Back to topTreatment
Before receiving treatment for TMDs, you should know:
- Sounds without pain in the temporomandibular joints are normal, happen frequently, and do not need treatment.
- Signs and symptoms of TMD go away in many people without treatment.
- Because evidence is lacking for the majority of TMD treatments, experts strongly recommend staying away from treatments that cause permanent changes to the jaw joints, teeth, or bite; or that involve surgery.
Nonsurgical Treatments
Because many jaw joint and muscle problems are temporary and do not get worse, simple treatment may be all that is necessary.
When you first feel discomfort in your jaw joints or muscles, your doctor or dentist may have you:
- Eat soft foods.
- Apply heat or cold to the face in combination with exercises to gently stretch and strengthen the jaw muscles.
- Take over-the-counter medications, for example nonsteroidal anti-inflammatory drugs (NSAIDs), like ibuprofen.
- Reduce habits such as jaw clenching, gum chewing, or nail biting.
If these steps do not help, or if in the process of trying them your doctor/dentist diagnoses a specific type of TMD, one or more of the following treatments may be recommended.
Physical Therapy
The goal of physical therapy is to maintain, improve, or bring back movement and physical function. There are several types of physical therapy. One type is manual therapy, in which a therapist uses his/her hands to stretch the soft tissues and muscles around the joint. Manual therapy has been shown to help improve function and relieve pain.
Self-management and Behavioral Health Approaches
Self-management refers to activities you can do yourself and include:
- Learn all you can about your specific type(s) of TMD.
- Learn meditation & relaxation techniques.
- Set specific goals related to managing your condition.
- Stay involved in activities that are meaningful to you.
Certain behavioral health approaches, usually offered by a psychologist, have been shown to help manage TMDs. These include cognitive behavioral therapy and biofeedback.
Cognitive behavioral therapy seeks to identify negative thoughts or thought patterns and change them, as well as provide coping skills.
Biofeedback involves using sensors that monitor breathing, heart rate, muscle contraction, and temperature. For example, a sensor on your jaw can detect when you tighten your jaw muscles. With the help of a therapist, you can learn to notice the unwanted behavior and relax.
Medications
Your doctor or dentist may recommend medication(s) to treat your symptoms.
These include:
- Over-the-counter medications such as:
- Nonsteroidal anti-inflammatory drugs (NSAIDs), used to treat pain.
- Prescription medications such as:
- Antianxiety medications.
- Antidepressants.
- Antiseizure medications.
- Opioids.
Some of these medications can lead to addiction or have other serious side effects. If you are prescribed any of these medications, make sure your doctor or dentist explains how to take them and for how long.
Intraoral Appliances
Intraoral appliances are devices that fit over the teeth. They do not change the teeth or bite. They are also known as nightguards, splints, stabilization appliances, occlusal splints, interocclusal splints, or bruxism splints.
There is not a lot of evidence they improve TMD pain. If a dentist or doctor suggests you use one:
- Make sure it is not designed to permanently change your bite.
- Stop using it and consult your dentist/doctor if it causes pain.
Complementary Treatments
A complementary treatment is a non-mainstream practice used together with conventional medicine. Acupuncture and transcutaneous electrical nerve stimulation (TENS) are two complementary treatments that have been studied for TMDs.
Acupuncture is a technique in which practitioners stimulate specific points on the body—most often by inserting thin needles through the skin. There is limited evidence that it helps TMDs.
TENS is a battery-powered device that uses electrodes placed on the skin. The device creates electrical impulses that may change how pain is perceived. Although some studies have shown that TENS may help relieve pain in TMDs and improve the ability to open the mouth, the studies were small with short-duration TENS treatments.
Surgery and Other Medical & Dental Procedures
The treatments discussed in this section are more complex, involve going into the chewing muscles or the temporomandibular joints (with a needle or other instrument), or changing your bite and teeth. More importantly, some of them – like occlusal treatments (see below)— don’t work and may make the problem worse. Before having any of these procedures:
- Ask about simpler treatments and try those first.
- Ask the doctor or dentist to explain the procedure—in detail—in a way you can understand.
- Ask how the procedure will help improve your specific TMD.
- Ask about the risks.
- Get second opinions from qualified medical or dental specialists.
Occlusal Treatments
Occlusion refers to how teeth fit together. For years it was thought that misaligned teeth (malocclusion) were a cause of TMDs; however, there is no evidence to support this belief. Occlusal treatments modify the teeth and bite. Examples include:
- Placing crowns on the teeth.
- Grinding down the teeth.
- Using orthodontic treatment(s) to change the position of some or all teeth.
There is no evidence these occlusal treatments work, and they could make the problem worse.
Botulinum Toxin
Botulinum toxin Type A works by relaxing muscles. It is FDA-approved for some medical conditions (like migraines) but not for TMDs. Studies have looked at injecting botulinum toxin Type A into the chewing muscles to reduce muscle spasm and pain. However, the information from these studies is limited and it is not clear whether this medication works to relieve TMD symptoms.
Prolotherapy
Prolotherapy involves injecting a solution into the TMJ area that causes irritation, with the goal of triggering the body to respond by repairing the joint. Prolotherapy has shown promise specifically for TMDs in which the joint is out of its normal position (dislocation) or when the joint goes beyond its normal range of movement (hypermobility). However, there have been only a few small studies on this treatment for TMDs.
Arthrocentesis
In this procedure a needle is used to push liquid into the TMJ. The pressure caused by the liquid removes scar-like tissue (adhesions). In addition, when the liquid is flushed out of the joint, it removes substances that cause inflammation. Arthrocentesis has been shown to help with pain relief and improve mouth opening in people whose temporomandibular disc is out of place; however, these effects do not last long.
Arthroscopy
During arthroscopy the doctor inserts an instrument with a tiny video camera into the jaw joint. The doctor can see the joint, which can help in diagnosis. He or she can also remove adhesions or reposition the joint’s disc. This procedure works moderately well in helping improve pain and function.
Surgery
Open surgery gives access to the temporomandibular joint through a cut (incision) next to the ear. It’s important to know that surgery makes permanent changes to your joint. There are no long-term research studies on the safety of open surgery for TMDs or on how well it works to relieve symptoms.
Surgery should only be considered if:
- There is destruction of the joint that cannot be fixed with other procedures.
- There are severe symptoms (pain and/or difficulty opening the mouth), despite trying other treatments.
If your healthcare provider suggests surgery, be sure to ask:
- Why are you suggesting surgery?
- Are there other options besides surgery?
- How will it help me?
- What are the risks?
TMJ Implants
Implants are artificial devices that are used to replace part of the jaw joint or the entire joint. There are currently three TMJ implants approved by the FDA.
Implants might be considered when:
- There is an injury to the joint.
- There is a condition you’re born with (congenital condition) that needs to be repaired.
- The joint is frozen (ankylosis), commonly caused by injury or infection.
- There’s severe damage to the joint.
- There’s ongoing pain.
- All simpler treatments have been tried and have failed.
Some studies suggest that, when used in very specific cases, TMJ implants can improve function and quality of life. As with any surgery, proceed with caution.
Implants used many years ago (and since taken off the market), did not help patients and left them with severe complications, including permanent damage to the jaw joint(s). Because of this, researchers have called for long-term studies to look at the safety and efficacy of the newer TMJ implants.
Remember: Before any surgery, including implant surgery, it is extremely important to get opinions from more than one doctor and to completely understand the risks. If possible, seek an opinion from a surgeon who specializes in treating TMDs.
Summary of Treatments for Temporomandibular Disorders (TMDs)
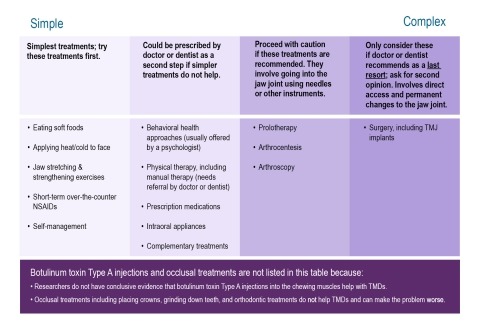
Helpful Tips
If you think you have a TMD or are diagnosed with one:
- Start with simple treatments first; remember that TMD symptoms often go away on their own, without treatment.
- Consult a dentist or doctor.
- Learn all you can about the TMD you have.
- Avoid (when possible) treatments that involve going into or permanently changing the jaw joints, especially surgery or TMJ implants.
- Understand all the risks when considering surgery or other medical or dental procedures that result in permanent change and seek an opinion from an orofacial pain clinic at a medical or dental school, if possible.
Additional Resources
- Temporomandibular Disorders and Jaw Pain
- MedlinePlus: Temporomandibular Joint Dysfunction
The NIH National Library of Medicine's collection of links to government, professional, and non-profit/voluntary organizations with information on temporomandibular disorders. - The TMJ Association
The TMJ Association is a non-profit, patient advocacy organization whose mission is to improve the quality of health care and the lives of everyone affected by temporomandibular disorders. - American Chronic Pain Association
The ACPA offers peer support and education in pain management skills to people with pain, their family and friends, and health care professionals.
Learn more about TMD clinical trials from NIDCR.
TMD (Temporomandibular Disorders) Research from NIDCR
November 2025
