Featured Updates

Explore NIDCR resources designed to support oversight, compliance, and excellence at every stage of your clinical research study

NIH is seeking public feedback on its proposed 2027–2031 Strategic Plan framework.
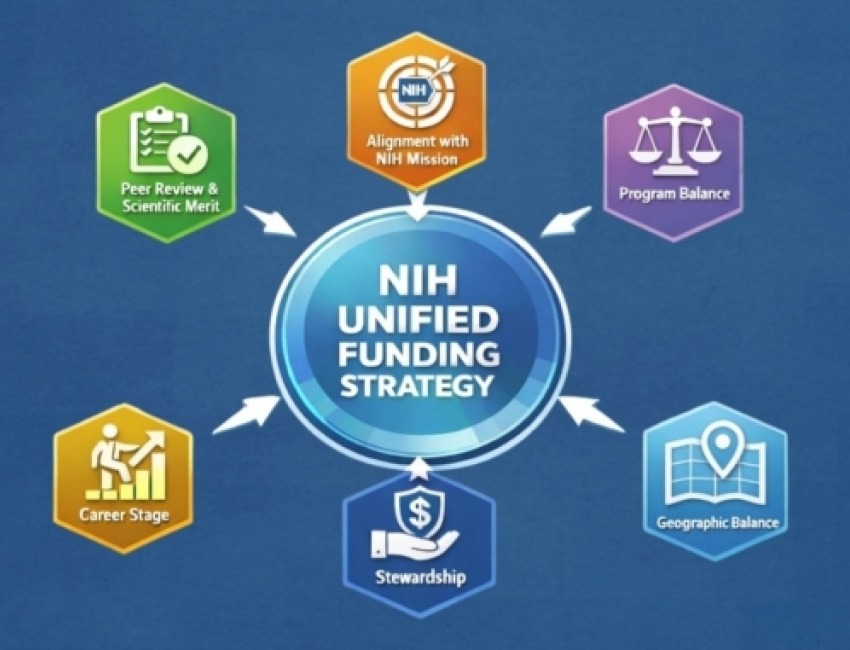
Learn more about NIH's new strategy for clear and consistent funding decisions across its Institutes and Centers

