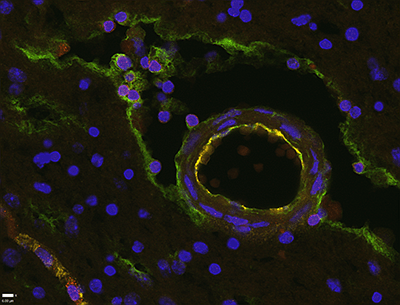
Brain Patrol
How our immune systems may be policing our brains
In Brief:
- NIDCR researchers and colleagues demonstrated the presence of lymphatic vessel cells and immune cells throughout the brains of humans.
- Their findings point to the existence of a lymphatic network that acts as a waste drainage system for the brain and may serve as a bidirectional conduit between the brain and immune system, a connection not thought to exist until recently.
You might say that NIDCR scientist Eva Mezey has had the brain on her mind for a very long time. Or to be more exact, the connection between the brain and the lymphatic system.
Growing up in post-World War II Hungary, Mezey was fascinated with her mother’s work as a medical researcher in a clinical lab at the Neurosurgical Institute of Budapest. Her mother filled Mezey’s childhood with her passion for scientific inquiry. “She became very interested in the cerebrospinal fluid, and she realized that she could help diagnose a variety of diseases based on a lumbar puncture,” Mezey recalls. “And she kept telling me as I was growing up that cerebrospinal fluid and lymphatics must be in connection with each other.”
For example, Mezey explains, her mother theorized that in cases when lung cancer first metastasized to the brain, the cancer had to be circulating through the lymphatic system, because in most cases it seemed to first appear on the same side of the brain as it had in the lung (if it was transported by the blood, she figured, its appearance in the brain would be randomized). It was not uncommon in the Mezey household for dinner table conversations, often in the presence of her mother’s colleagues, to cover how the cranial nerves leave the cranial vault, or the vagaries of the peripheral lymphatics. In time, the young Mezey would offer her own theories on how it all worked.
Later as a researcher, Mezey took her work in different directions, and unlocking the mysteries of the lymphatic system was left to others. That is until 2015, when she read about a study in mice that demonstrated the presence of lymphatic vessels in the membranes that cover the brain’s surface. There it was: evidence that supported her mother’s hypothesis from so many years ago. The paper piqued her interest on another level, in that she wanted to explore the work that she knew had preceded it, including the science conducted by her mother’s colleagues decades earlier in Hungary.
“I got in touch with my old mentor, a relationship that began some 50 years ago, and I told him, ‘Look, I really want to do this study. Are you interested in helping me?’” Mezey recalls. That man, Miklós Palkovits, MD, PhD, DSc, is “one of the best neuroanatomists in the world,” according to Mezey, and he came back with an emphatic “yes.”
Palkovits happens to run a brain tissue bank affiliated with a forensic medicine program in Hungary. Which was fortuitous given what came next. In looking at the literature on the lymphatic system from across the years, Mezey was struck by the Hungarian researchers’ observations in animals that tying off lymphatic vessels in the neck caused the brain to swell. As Mezey explains, “It is a clear sign that there must be liquid output from the brain that is shut down.”
As morbid as it may sound, Palkovits wondered what they would find if they examined brain tissue from donors who had died of strangulation, which would presumably cut off outflow into the lymphatic vessels in the neck. Would they discover evidence that the lymphatic system was, in fact, at work in the brain? The answer was “yes.” In fact, they found that T cells—white blood cells that play a critical role in immune responses—had piled up within the brain above the point of strangulation, their exit from the brain suddenly blocked.
Throughout the brains of these and other donors, the team demonstrated the presence of cells similar to those that make up lymphatic vessels outside the brain. These so-called endothelial cells were found, often in close proximity to T cells, along blood vessels; around and within nerve bundles in the brain; and in the membranes covering the brain. T cells were particularly abundant along and throughout the trigeminal nerve, which conveys motor signals and sensation to and from the face and mouth.
According to Mezey and her colleagues, these findings point to the presence of a network of lymphatic spaces that carry waste out of the brain along and within the walls of blood vessels and along cranial nerves, including the trigeminal nerve, and into the lymph nodes of the neck.
The implications are significant, says Mezey. For years the immune system’s reach was thought not to extend into the brain; in other words, whereas the immune system reacted to problems detected throughout the body, the brain remained largely unpoliced by patrolling T cells. Mezey’s and Palkovits’ discovery—which encompassed over five years of work—suggests otherwise.
There’s still much to be done to fully understand this system in the human brain, says Mezey. “But potentially the implication is that the presence of a lymphatic system in the brain could help explain the pathology of certain brain diseases.”
She is already moving forward with more research, but she says it’s important to recognize that scientific work today would not be possible without what happened before. A theory proffered, perhaps, over a dinner of Hungarian goulash five decades ago, for example, can inspire discovery for generations.
Reference
An immunohistochemical study of lymphatic elements in the human brain. Mezey E, et al. Proc Natl Acad Sci U S A. 2021 Jan 19;118(3):e2002574118. doi: 10.1073/pnas.2002574118. PMID: 33446503.
Attention Editors
Reprint this article in your own publication or post to your website. NIDCR News articles are not copyrighted. Please acknowledge NIH's National Institute of Dental and Craniofacial Research as the source.
October 2024