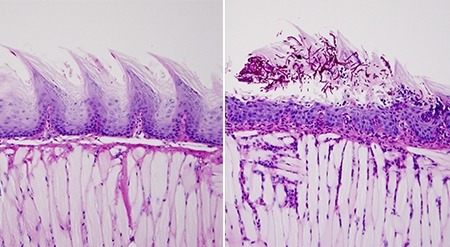
How Fungus Finds a Foothold in the Mouth
Overactive immune response leaves tissues vulnerable to infection in rare disease
As a key point of entry into the body, your mouth is an important gatekeeper that protects against harmful foreign invaders. The mucous membrane lining the inside of the mouth—the oral mucosa—is home to immune cells that monitor the surroundings for potentially infectious microbes and other pathogens. Imbalances in these immune responses can lead to disease, including fungal infections. A recent study by a team that included NIDCR scientists adds an unexpected twist to what was known about the immune disturbances that allow fungus to take hold in the body’s mucosal tissues, such as the mouth.
The team, led by Michail Lionakis, MD, ScD, from NIH’s National Institute of Allergy and Infectious Diseases, studied the oral mucosal tissues of people and mice with genetic defects that cause a rare autoimmune disease with wide-ranging effects on the body, including chronic infections of the mucous membranes with the yeast fungus Candida. In humans, the condition is called APECED, or autoimmune polyendocrinopathy-candidiasis-ectodermal dystrophy.
“Because the mouth is easy to access and biologically similar to mucosal tissues throughout the body, it’s an obvious site to study mechanisms of disease,” says NIDCR immunologist Niki Moutsopoulos, DDS, PhD, who is a senior author on the paper. “Studying how rare immune diseases affect the mouth can reveal general insights about the immune system and lead to better interventions for both rare and common diseases of the mouth and elsewhere in the body.”
Previous work by Moutsopoulos and others focused on immune cells called T-helper 17 cells, which normally protect the mouth from fungal and other infections by producing a signaling molecule called interleukin-17 (IL-17). Disruptions in this protective IL-17 immune response can increase humans’ and animals’ susceptibilities to mucosal fungal infections.
However, in the context of APECED, the NIH team found that oral fungal infections arose even though IL-17 mucosal immune responses were intact. Instead, the researchers found, the infections emerged due to an overactive response by a different set of immune cells, called Type 1 T-cell immunity. The discovery of this abnormal immune response could lead to better therapies for fungal infections in patients with APECED and other diseases and adds to our knowledge about the immune mechanisms at play in the mouth and other mucosal tissues.
For more details about the study, visit the NIAID Now Blog post, How Do Fungal Infections Take Hold? Rare Disease Offers New Insights.
Reference
Aberrant type 1 immunity drives susceptibility to mucosal fungal infections. Break TJ, Oikonomou V, et al. Science, 371, 252 (2021). PMID: 33446526.
NIH Support: Support for this research came from the intramural and extramural research programs of NIDCR and NIAID, as well as the intramural programs of the National Cancer Institute, the National Institute of Diabetes and Digestive and Kidney Diseases, and the National Institute on Deafness and Other Communication Disorders.
Attention Editors
Reprint this article in your own publication or post to your website. NIDCR News articles are not copyrighted. Please acknowledge NIH's National Institute of Dental and Craniofacial Research as the source.
November 2024