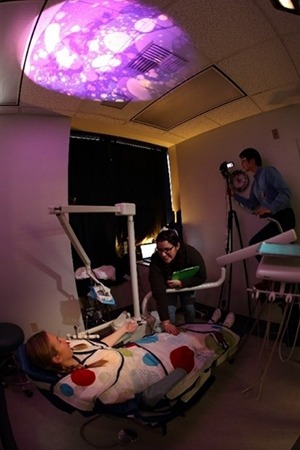
A Safe Space in the Dental Clinic
Multidisciplinary teams create soothing dental environments for children with autism
When it’s time for your regular dental visit, you know the drill—you lie in the vinyl chair and breathe in the disinfectant-scented air as the hygienist shines the light on your mouth and switches on the high-pitched cleaning tool. For many of us, the sensory environment of the dental clinic is familiar and routine. But for children with autism spectrum disorder (ASD), the sensations can be overwhelming, making it hard to receive regular dental care and putting them at risk for poor oral health.
“Dental clinic visits can be incredibly taxing for the child, the parent, and the dental practitioner,” says Dominique Como, an occupational therapist and NIDCR-supported PhD student from the University of Southern California (USC). “I want to find ways to make this a better experience for everyone.”
With NIDCR support, Como and her colleagues are evaluating sensory adaptations to the dental environment that can help to reduce anxiety in children with ASD. The research seems especially timely, because ASD appears to be on the rise. Since 2000, the prevalence of ASD has climbed from 1 in 150 to 1 in 54 children in the US, indicating that a growing number of dental practitioners are encountering these patients. However, studies have shown that many dental providers feel unqualified to work with patients with special needs.
Como and colleagues lay out suggestions for addressing these challenges in a recent review article featured on the online cover of a special issue of the International Journal of Environmental Research and Public Health. The strategies described in the article provide a blueprint for reducing dental treatment barriers for ASD patients. The article makes the case for collaborations among dental clinicians and specialists such as occupational therapists, who can contribute their expertise and help dental providers learn to identify and accommodate ASD patients’ needs.
Citing their own NIDCR-supported study at USC as an example, the authors describe how interdisciplinary teams are creating a sensory-friendly experience for children with ASD. Strategies such as removing bright lights and loud noises, adding calming music, and covering children with a weighted blanket that simulates a firm hug can be calming and help prevent sensory overload.
New environments and unpredictable situations can also distress children with ASD. For their study, the USC team developed a social story with real-life photographs of a child receiving care in the dental clinic. Before a visit, parents were asked to read the stories to their children to help them prepare for the upcoming dental activities. Visual aids that break down procedures step-by-step may also help children with ASD prepare for dental visits.
While Como and her colleagues are still evaluating the strategies’ effectiveness, families have described the interventions positively and reported some success in enhancing their children’s oral care. Como also encourages clinicians to seek the expertise of parents, who can help tailor strategies to their child’s unique needs.
“Interdisciplinary collaboration can bring numerous insights,” says Como. “So many factors of our health are interconnected—our interventions should be as well.”
Related Links
Reference
Oral Health and Autism Spectrum Disorders: A Unique Collaboration between Dentistry and Occupational Therapy. Como DH, Stein Duker LI, Polido JC, Cermak SA. Int J Environ Res Public Health. 2020 Dec 27;18(1):135. doi: 10.3390/ijerph18010135. PMID: 33375475; PMCID: PMC7795681.
Attention Editors
Reprint this article in your own publication or post to your website. NIDCR News articles are not copyrighted. Please acknowledge NIH's National Institute of Dental and Craniofacial Research as the source.
September 2024